Abstract
Objective
Arthroscopic shoulder surgery (ASS) is often followed by severe pain. Interscalene brachial plexus block (ISB) was used to relieve such pain. The aim of the study was to compare the effect of adding either dexamethasone or ketamine to ISB on time to the fi rst request for analgesia.
Methods
Sixty patients scheduled for ASS were enrolled in this study. Before induction of general anaesthesia, patients were randomly allocated to two groups; in Group D, patients received ISB with bupivacaine 0.3%, 5 mL lidocaine 2% plus 8 mg dexamethasone. Whereas in Group K, patients received ISB with bupivacaine 0.3%, 5 mL lidocaine 2% plus 50 mg ketamine. Time to the fi rst administration of supplemental analgesic postoperative was our primary concern. Secondary outcomes included pain score, patient satisfaction, and side effects of either block or drugs. Student’s t-test was utilized for comparison between the two groups. Chi-square test was used to test the association between categorical variables.
Results
Time to the first request of analgesia was statistically significantly longer in Group D when compared to Group K. The onset of sensory and motor blocks, number of patients requiring rescue analgesia and patient satisfaction showed no difference between the two groups. Pain score in Group K, compared to Group D, was statistically signifi cant less early postoperatively.
Conclusions
We conclude that addition of dexamethasone to local anesthetic in ISB for patients undergoing ASS resulted in longer time elapsed to the first request of analgesia when compared with ketamine. Pain score in the early postoperative period was statistically improved in ketamine group, but this might be of no clinical signifi cance, when compared with dexamethasone.
Keywords
arthroscopic shoulder surgery ; interscalene ; dexamethasone
Introduction
Arthroscopic shoulder surgery (ASS) is often followed by severe pain. Many modalities have been postulated to relieve such pain. These modalities include interscalene brachial plexus block (ISB), suprascapular nerve block and intra-articular local anesthetic injection.1
The use of an ISB in addition to general anaesthesia permits control of respiration safely, and maintenance of surgical analgesia easily.2 Also, this technique resulted in higher patient satisfaction with lower narcotic requirements either during or shortly after the surgery.3 Single-injection ISB is effective but time-limited to combat pain after shoulder surgery.4 Various adjuvants, like dexamethasone, have been used to prolong the time of pain relief in ASS performed under ISB.5
Intravenous intraoperative low-dose ketamine has been used to decrease acute postoperative pain following ASS.6 The primary concern of this study was a comparison of the first request of analgesia after ISB containing either dexamethasone or ketamine as an additive in patients undergoing ASS between. The secondary goals were pain score, patient satisfaction, and side effects.
Methods
After informed consent and institutional research board approval, 60 patients, ASA (American Society of Anesthesiologists physical status classification) I or II, subjected to ASS were randomized to two groups. In the first group, patients received ISB with bupivacaine 0.3% plus 8 mg dexamethasone (Group D). Whereas in other group patients received ISB with bupivacaine 0.3% plus 50 mg ketamine (Group K). The total volume of the block was 25 mL including 15 mL bupivacaine 0.5%, 5 mL lidocaine 2% plus 5 mL normal saline containing either ketamine or dexamethasone. The study was started in a university hospital from July 2016 and ended in January 2017. Criteria for exclusion from the study include epilepsy, diabetes, obstructive pulmonary disease, muscular disease, bleeding diathesis, and a history of allergy to the drugs used in this study. A computer-generated method was used for randomization. The block solutions looked identical and were prepared by a pharmacist who is blinded to the other personnel involved in the block as well as to the patients. Assessment of postoperative parameters was done by personnel blinded to the study. All cases were blocked by same anesthetist. The all surgeries were done by same surgeon team. The ISB was given before induction of general anesthesia (GA) guided by SonoSite portable ultrasound unit (SonoSite, Bothell, WA, USA).
After identification of the sternocleidomastoid muscle and interscalene groove at the approximate level of C6, a linear transducer is placed 90° to the course of the interscalene muscles. The brachial plexus at this level appeared as three to five hypoechoic circles. The carotid artery and internal jugular vein may be seen lying anterior to the anterior scalene muscle. After careful aspiration for nonappearance of blood, local anesthetic (hypoechoic) spread occurred adjacent to the plexus.7,8 The block was assessed to be well established before induction of anesthesia.
After a period of preoxygenation with 100% oxygen, GA was induced with propofol and cisatracurium. Then, anesthesia was maintained with sevo flurane, nitrous/oxygen. Intraoperative monitoring included electrocardiogram (ECG), heart rate, pulse oximetry, non-invasive blood pressure, and end-tidal carbon dioxide concentration. A pinprick test was mean to test the sensory block (whereas normal sensation = 0; loss of sensation of pin prick = 1 and loss of sensation to touch = 2). Shoulder movement was the way to test motor block (normal movement = 0; paresis = 1 and lack of movement = 3). Time passed from giving local anesthetic till loss of sensation of pinprick performed every minute (sensory score = 1) was the onset of sensory block, whereas time passed from giving local anesthetic till absent movement (motor score = 2) was the onset of motor block. All surgeries were performed by the one surgeon. Postoperative pain was assessed using a visual analog scale (VAS) (no pain = 0 cm and the worst pain imaginable = 10 cm) at 2, 4, 6, 8, 12, and 24 hours, postoperatively. Patients were discharged from the postanesthetic care unit when Aldrete’s score was not less than 9.9 Time to the first administration of supplemental analgesic postoperative was our primary concern. If pain more than 3, rescue analgesic was intravenous tramadol 1 mg/kg. Secondary outcomes included pain score, patient satisfaction as percentage (0% = not satisfied, 100% = fully satisfied), side effects of either block (arm numbness, arm weakness, phrenic nerve palsy, Horner syndrome, and dyspnea) or drugs (hallucination, nausea, and vomiting).
Based on pilot study and using the t-test and setting α to 0.05, we needed minimally 25 cases in each group to detect 15% difference in time to the first request of analgesia (primary goal) with 80% power. We increased the sample to 30 cases to compensate for possible dropouts. Statistical Package of Social Science (SPSS) program for Windows (Standard version 22.0; IBM Corp., Armonk, NY, USA) was used for analysis of collected data. The normality of data was primarily tested with the one-sample Kolmogorov–Smirnov test. Chi-square test was used to test the association between categorical variables. When expected cell count less than 5, Fischer’s test was used. Continuous variables were presented as mean ± standard deviation (SD). Number and percent were used to describe qualitative data. Student’s t-test was utilized for comparison between the two groups. When p value was less than or equal to 5%, the results were considered significant. The smaller the p value, the more significant are the results.
Results
Seventy patients, submitted for arthroscopic shoulder surgeries, were assessed for eligibility; out of the 70 patients, 60 patients completed this study. Ten patients were excluded because of obstructive pulmonary disease, diabetes, epilepsy, and patient’s refusal (Fig. 1).
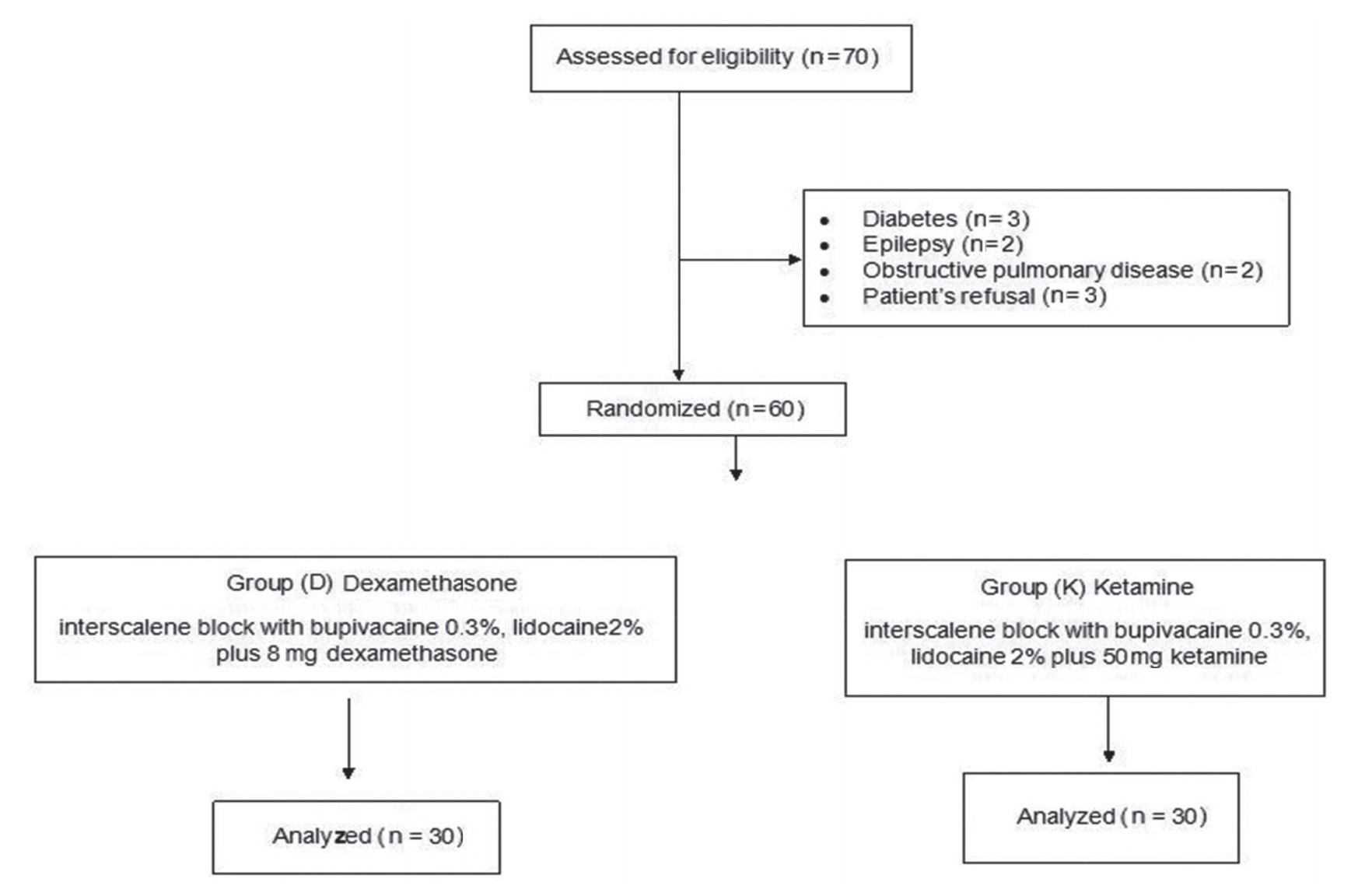
Download full-size image
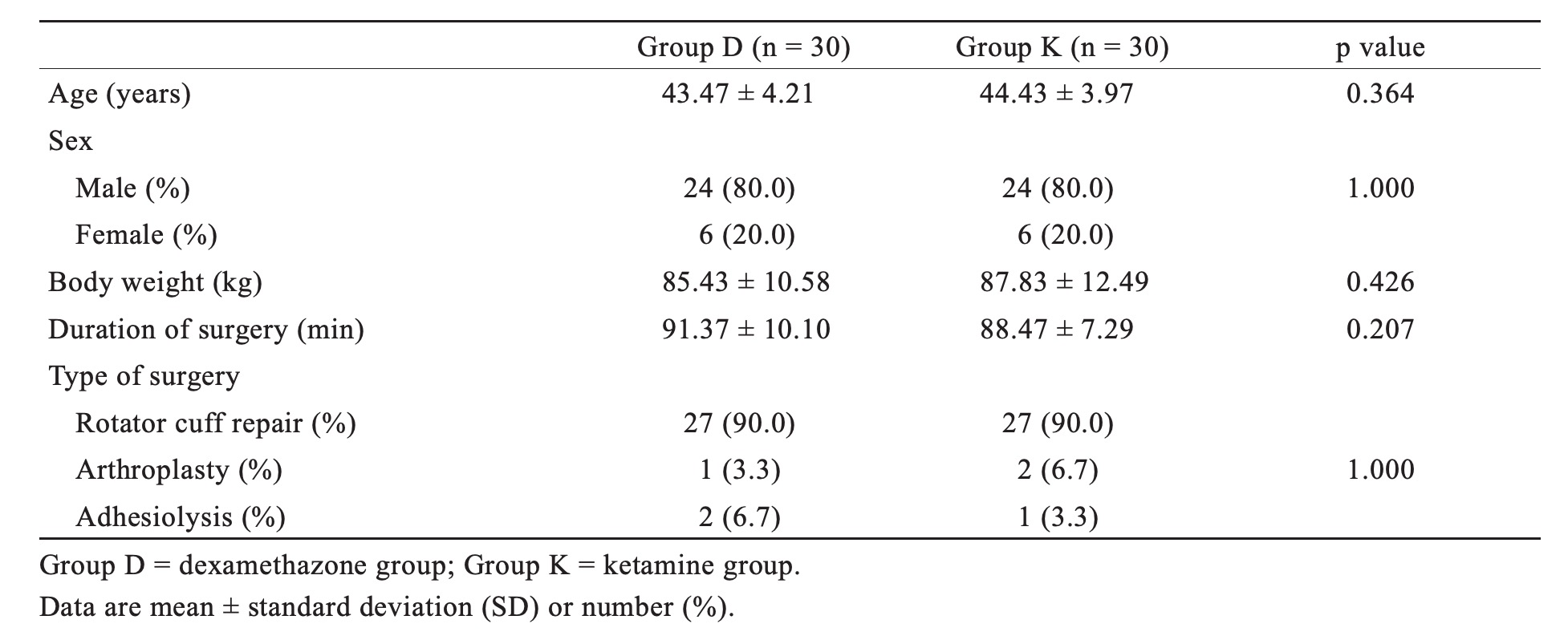
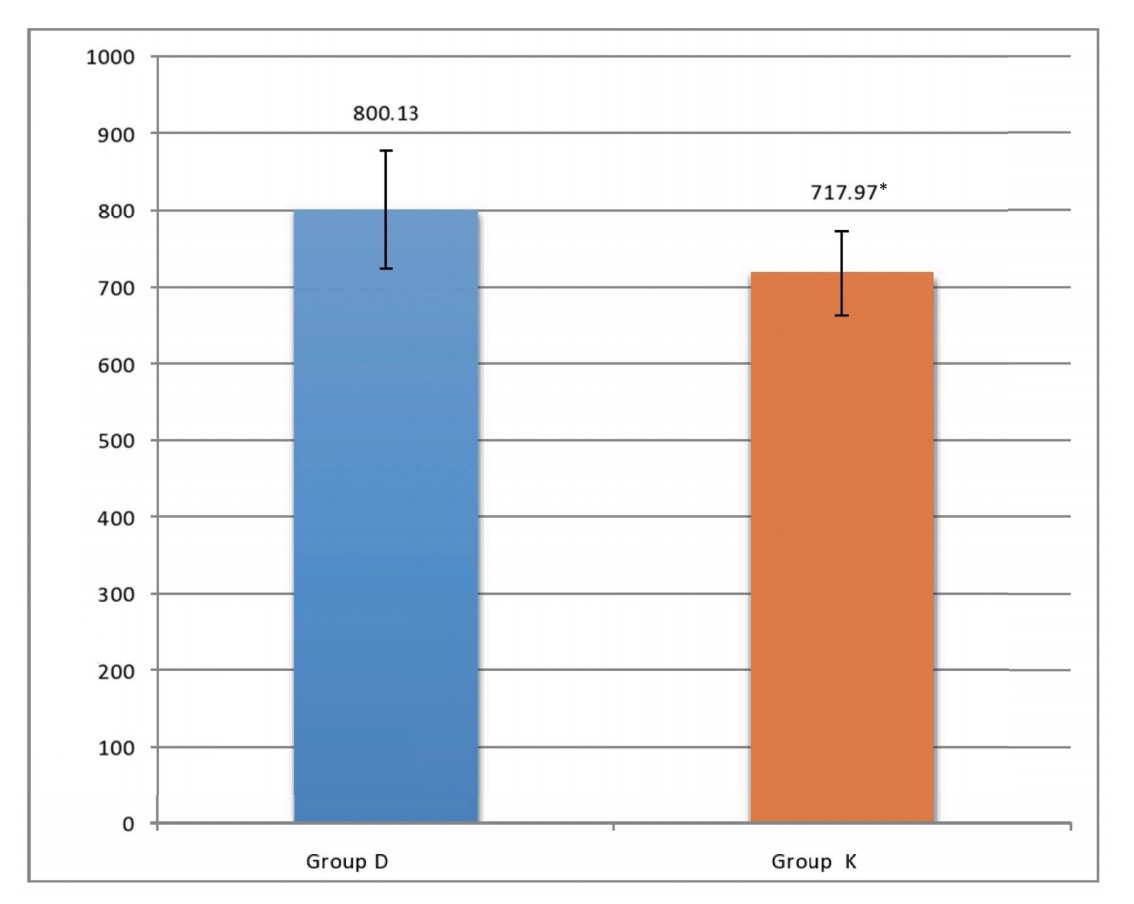
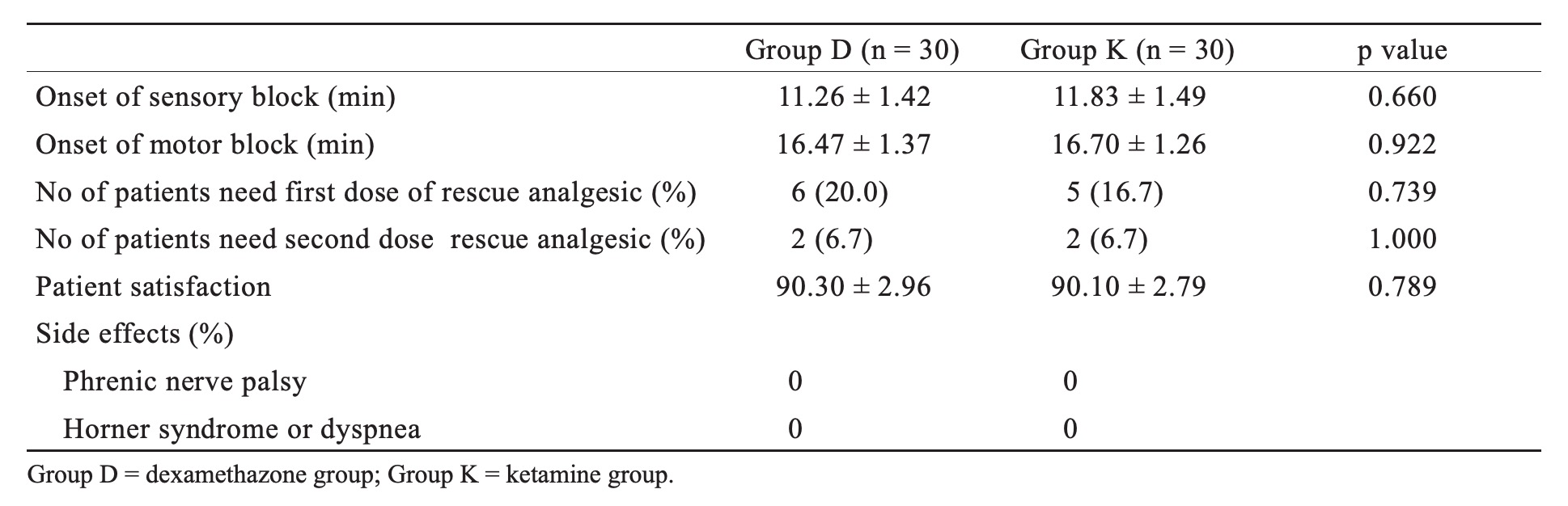
Patients showed no statistically significant difference with respect to patients’ age, sex, weight, duration of surgery, and type of surgery (Table 1). Time to the first request of analgesia was statistically significantly longer in Group D when compared to Group K (Fig. 2). The onset of sensory and motor blocks, number of patients requiring rescue analgesia, and patient satisfaction showed no difference between the two groups (Table 2).
Download full-size image
Download full-size image
Group D = dexamethazone group; Group K = ketamine group.
*Highly signifi cant p < 0.001.
Download full-size image
Download full-size image
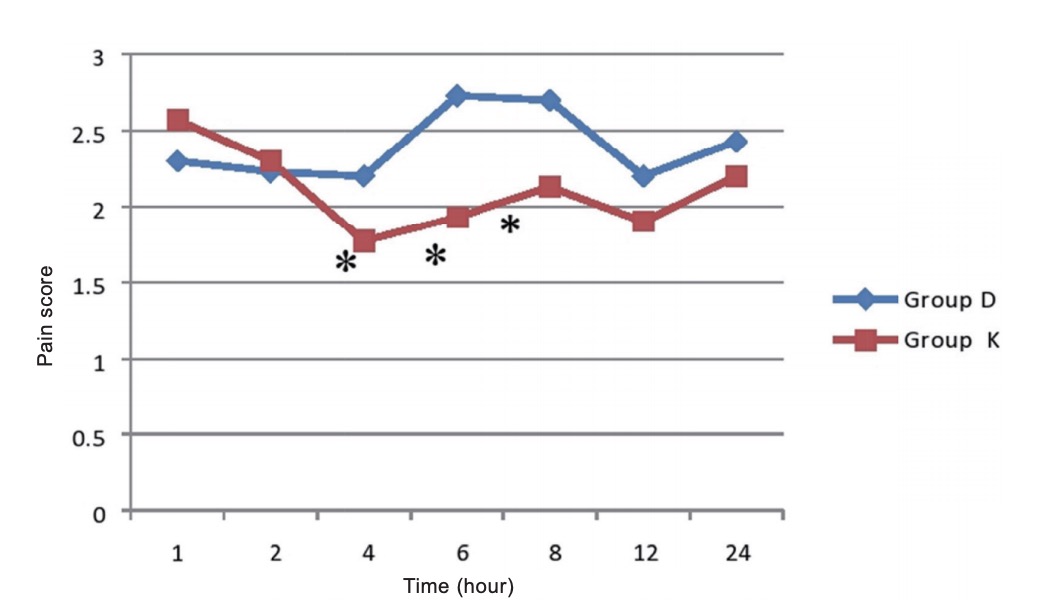
Group D = dexamethazone group; Group K = ketamine group.
*Signifi cant when compared to other group.
Discussion
Shoulder arthroscopic surgeries have been associated with the frequent occurrence of severe pain after surgery. Improper management of such pain might result in delayed recovery and rehabilitation. Use of regional analgesia in addition to GA decreases requirements of anesthetics during surgery and provides a better quality of pain control after surgery.1
Interscalene nerve block has been used frequently to control pain after shoulder surgery. Although single-injection block is effective, it has the disad-vantage of limited duration. GA along with ISB have been utilized for shoulder surgery,10 with a target of better maintenance of surgical analgesia, higher patient satisfaction with a decreased need for analgesics either during or after surgery.11
In a double-blinded study, Cummings et al. found that dexamethasone prolongs analgesia from single-injection ISB. In this study, the results were the same regardless the used local anesthetic, ropivacaine or bupivacaine.4
Prolongation of regional anesthesia with dexamethasone attributed to increasing the efficiency of potassium channels on nociceptive C-fibers, vasoconstriction, and reduction of local anesthetic absorption. Potassium channels have an inhibitory effect on C-fibers transmitting pain.12,13
In this study, the onset of sensory and motor blocks was faster in dexamethasone group than in ketamine group but the difference was not statistically significant.
Ketamine, in a dose of 50 mg, has been added to local anesthetic aiming to prolong the axillary brachial plexus block or epidural anesthesia as a result of the direct action on the nerve root fi bers.14,15 Also, Clerc et al. found that addition of 75 mg ketamine to bupivacaine 0.5% in inguinal field block after hernia repair resulted in minimal improvement in the analgesic effect of bupivacaine. They explained such effect by low pain level after tension-free hernia surgery.16
Many studies discussed the utility of adding ketamine to the peripheral nerve block especially brachial plexus block. Some studies reported decreased severity of postoperative pain and requirement for analgesics, without significant adverse effects with addition of ketamine.17,18
This study showed that the pain score in the early postoperative period was statistically improved in ketamine group when compared with dexamethasone. However, such difference might be of no clinical significance as the number of patients requiring rescue analgesia in both groups was comparable.
In contrast to this finding, Senel et al.19 found that ketamine did not result in augmentation of the local anesthetic effect at the level of the axillary brachial plexus nerve roots. Also, it did not enhance postoperative analgesia with the dose of 50 mg when combined with ropivacaine. They stated that the low concentration of 50 mg ketamine in a volume of 40 mL might be the cause and a higher concentration of ketamine is necessary for ketamine to be used as an adjuvant to local anesthetics in brachial plexus block.
Adding ketamine to local anesthetic in epidural analgesia resulted in favorable results20 but much less variable results noticed with peripheral nerve blocks.21 The reason for using ketamine as an adjunct to local anesthetics is the local anesthetic-like action that ketamine has.Lee et al.22 have noticed no prolongation of sensory and motor effects of ketamine when added to ropivacaine 0.5% in ISB. They explained that by two assumptions. First, low concentration of ketamine in their study (0.1%) which is not enough to exert its local anesthetic action. Secondly, the local antinociceptive effect of ketamine is valid only when there is an inflammatory process at the site of injection. The third explanation was assumed by Omar et al.,23 is the availability of ketamine at the site of injection. Ketamine (0.5 mg/kg in Omar et al. study and 50 mg in our study) might have been absorbed quickly in the systemic circulation and any local anesthetic effect could have been masked specially with bupivacaine.
Noyan24 reported that ketamine was not sufficient to provide adequate duration of analgesia when added to axillary block in hand surgery. Meanwhile local anesthetic together with ketamine had a better anesthesia time. Ketamine might increase the binding capacity of local anesthetic to albumin alpha acid glycoprotein.
In a randomized study, Lashgarinia et al.25 concluded that addition of ketamine to local anesthetic in the brachial plexus block could decrease the severity of pain and requirement for analgesia after surgery without improvement in the onset and duration of the sensory or motor block. The block in this study was guided by ultrasound. The authors considered ketamine as an alternative for augmentation of the analgesic action of local anesthetic in the brachial plexus block. Hong et al.26 concluded that use intravenous ketamine before surgery did not decrease scores of pain after arthroscopic rotator cuff repair or fentanyl consumption during surgery with intra-articular local anesthetic injection. However, results might differ with different routes of ketamine administration.
Although ketamine resulted in improved pain score in the early postoperative period, but this might be of no clinical significance, as the number of patients requiring first or second dose of rescue analgesia and patient satisfaction showed no difference between the two groups.
Adverse effects reported with ISB include phrenic nerve palsy and Horner syndrome. ISB is associated with cranial nerve paresis in very rare cases.27
The present study showed no complication associated with ISB for patients undergoing shoulder arthroscopy, as the block is ultrasound-guided. Many studies showed similar results.28
One of the limitations to this study is the absence of control group with local anesthetic without additive as the effect of dexamethasone as an additive to ISB has been proved by metanalysis and our aim is to find out the comparative effect of ketamine. Further studies with a different dose or prolonged use of ketamine in a larger population may show different results.
Conclusion
We conclude that addition of dexamethasone to local anesthetic to ISB for patients undergoing ASS resulted in longer time elapsed to the first request of analgesia when compared with ketamine. Pain score in the early postoperative period was statistically improved in ketamine group, but this might be of no clinical significance, when compared with dexamethasone.
References
| 1 |
Kumara AB, Gogia AR, Bajaj JK, Agarwal N.
Clinical evaluation of post-operative analgesia comparing suprascapular nerve block and interscalene brachial plexus block in patients undergoing shoulder arthroscopic surgery.
J Clin Orthop Trauma 2016;7:34–39.
|
| 2 |
Zoremba M, Kratz T, Dette F, Wulf H, Steinfeldt T, Wiesmann T.
Supplemental interscalene blockade to general anesthesia for shoulder arthroscopy: effects on fast track capability, analgesic quality, and lung function.
Biomed Res Int 2015;2015:325012.
|
| 3 |
Ozturk L, Kesimci E, Albayrak T, Kanbak O.
Bispectral index-guided general anesthesia in combination with interscalene block reduces desflurane consumption in arthroscopic shoulder surgery: a clinical comparison of bupivacaine versus levobupivacaine.
BMC Anesthesiol 2015;15:104.
|
| 4 |
Cummings KC 3rd, Napierkowski DE, Parra-Sanchez I, et al.
Effect of dexamethasone on the duration of interscalene nerve blocks with ropivacaine or bupivacaine.
Br J Anaesth 2011;107:446–453.
|
| 5 |
Jadon A, Dixit S, Kedia SK, Chakraborty S, Agrawal A, Sinha N.
Interscalene brachial plexus block for shoulder arthroscopic surgery: prospective randomized controlled study of effects of 0.5% ropivacaine and 0.5% ropivacaine with dexamethasone.
Indian J Anaesth 2015;59:171–176.
|
| 6 |
Woo JH, Kim YJ, Baik HJ, Han JI, Chung RK.
Does intravenous ketamine enhance analgesia after arthroscopic shoulder surgery with ultrasound-guided single-injection interscalene block?: a randomized, prospective, double-blind trial.
J Korean Med Sci 2014;29:1001–1006.
|
| 7 |
Vieira PA, Pulai I, Tsao GC, Manikantan P, Keller B, Connelly NR.
Dexamethasone with bupivacaine increases duration of analgesia in ultrasound-guided interscalene brachial plexus blockade.
Eur J Anaesthesiol 2010;27:285–288.
|
| 8 |
Casati A, Fanelli G, Albertin A, et al.
Interscalene brachial plexus anesthesia with either 0.5% ropivacaine or 0.5% bupivacaine.
Minerva Anestesiol 2000;66:39–44.
|
| 9 | |
| 10 |
Bosco L, Zhou C, Murdoch JAC, et al.
Pre- or postoperative interscalene block and/or general anesthesia for arthroscopic shoulder surgery: a retrospective observational study.
Can J Anaesth 2017;64:1048–1058.
|
| 11 |
Borgeat A, Dullenkopf A, Ekatodramis G, Nagy L.
Evaluation of the lateral modified approach for continuous interscalene block after shoulder surgery.
Anesthesiology 2003;99:436–442.
|
| 12 |
Choi S, Rodseth R, McCartney CJL.
Effects of dexamethasone as a local anaesthetic adjuvant for brachial plexus block: a systematic review and meta-analysis of randomized trials.
Br J Anaesth 2014;112:427–439.
|
| 13 |
Lim D, Gold CM.
Intravenous dexamethasone for prolonged duration of axillary nerve blockade.
AANA J 2017;85:189–194.
|
| 14 |
Loix S, De Kock M, Henin P.
The anti-inflammatory effects of ketamine: state of the art.
Acta Anaesthesiol Belg 2011;62:47–58.
|
| 15 |
Sethi M, Sethi N, Jain P, Sood J.
Role of epidural ketamine for postoperative analgesia after upper abdominal surgery.
Indian J Anaesth 2011;55:141–145.
|
| 16 |
Clerc S, Vuilleumier H, Frascarolo P, Spahn DR, Gardaz JP.
Is the effect of inguinal field block with 0.5% bupivacaine on postoperative pain after hernia repair enhanced by addition of ketorolac or S(+) ketamine? Clin J Pain 2005;21:101–105.
doi:10.1097/00002508-200501000-00012
|
| 17 |
Sabra MM, Fadlallah BI, Saleh AA, Alkomeyty A, Alkenany H.
Dexmedetomidine versus ketamine as an adjuvant in ultrasound-guided axillary brachial plexus block.
AAMJ 2014;12(Suppl 1):110–126.
|
| 18 |
Tverskoy M, Oren M, Vaskovich M, Dashkovsky I, Kissin I.
Ketamine enhances local anesthetic and analgesic effects of bupivacaine by peripheral mechanism: a study in postoperative patients.
Neurosci Lett 1996;215:5–8.
|
| 19 |
Senel AC, Ukinc O, Timurkaynak A.
Does the addition of tramadol and ketamine to ropivacaine prolong the axillary brachial plexus block? Biomed Res Int 2014;2014:686287.
doi:10.1155/2014/686287
|
| 20 |
Tan PH, Kuo MC, Kao PF, Chia YY, Liu K.
Patient-controlled epidural analgesia with morphine or morphine plus ketamine for post-operative pain relief.
Eur J Anaesthesiol 1999;16:820–825.
|
| 21 |
Meurant F, Colling E, Welter J, Koch JP, Merle M.
Effect of clonidine, tramadol, and s(+)-ketamine as adjuvants in brachial plexus anesthesia using ropivacaine versus levobupivacaine.
Can J Anesth 2006;53(Suppl 1):24137.
|
| 22 |
Lee IO, Kim WK, Kong MH, et al.
No enhancement of sensory and motor by ketamine added to ropivacaine interscalene brachial plexus blockade.
Acta Anaesthesiol Scand 2002;46:821–826.
|
| 23 |
Omar AM, Mansour MA, Abdelwahab HH, Aboushanab OH.
Role of ketamine and tramadol as adjuncts to bupivacaine 0.5% in paravertebral block for breast surgery: a randomized double-blind study.
Egypt J Anaesthesia 2011;27:101–105.
|
| 24 |
Noyan A.
On effects of ketamine to axillary block in hand surgery.
J Reconstr Microsurg 2002;18:197.
|
| 25 |
Lashgarinia M, Naghibi K, Honarmand A, Safavi M, Khazaei M.
Effect of ketamine as an adjuvant in ultrasound-guided supraclavicular brachial plexus block: a double-blind randomized clinical trial study.
Adv Biomed Res 2014;3:232.
|
| 26 |
Hong EP, Jeong DH, Kang HY, Choi JH, Park SW.
The effect of preemptive intravenous ketamine on postoperative pain in patients undergoing arthroscopic rotator cuff repair with intra articular ropivacaine injection.
Anesth Pain Med 2016;11:71–75.
|
| 27 |
Chiaghana CO, Awoniyi CA.
Delayed onset and long-lasting hemidiaphragmatic paralysis and cranial nerve deficit after interscalene nerve block for rotator cuff repair in beach chair position.
J Clin Anesth 2016;34:571–576.
|
| 28 |
Singh A, Kelly C, O’Brien T, Wilson J, Warner JJ.
Ultrasound-guided interscalene block anesthesia for shoulder arthroscopy: a prospective study of 1319 patients.
J Bone Joint Surg Am 2012;94:2040–2046.
|