Outline
Abstract
Background: Reducing anesthesia-controlled time (ACT) such as extubation time may improve operation room (OR) efficiency result from different anesthetic techniques. However, the information about the difference in ACT between desflurane (DES) anesthesia and propofol-based total intravenous anesthesia (TIVA) techniques for open liver resection under general anesthesia is not available in the literature.
Methods: This retrospective study uses our hospital database to analyze the ACT of open liver resection after either DES/fentanyl-based anesthesia or TIVA via target-controlled infusion (TCI) with fentanyl/propofol from January 2010 to December 2011. The various time intervals including waiting for anesthesia time, anesthesia time, surgical time, extubation time, exit from OR after extubation, total OR time, and post-anesthetic care unit stay time and percentage of prolonged extubation (≥ 15 minutes) were compared between the two anesthetic techniques.
Results: We included 143 hepatocellular carcinoma patients, with 82 patients receiving TIVA and 61 patients receiving DES. The extubation time was faster (10.1 ± 3.2 min vs. 11.8 ± 5.2 min; P = 0.03), and the incidence of prolonged extubation was lower (9.8% vs. 26.8%; P = 0.02) in the DES group than in the TIVA group. The factors contributed to prolonged extubation were age, sex, anesthetic technique, and anesthesia time.
Conclusion: The DES anesthesia provided faster extubation time and lower incidence of prolonged extubation compared with propofol-based TIVA by TCI in elective open liver resection. Besides, older age, male, TIVA, and lengthy anesthesia time were factors affecting prolonged extubation.
Keywords
anesthesia-controlled time, desflurane, open liver resection, propofol, target-controlled infusion
Introduction
Anesthesia-controlled time (ACT) is one of the most important factors that regulate operating room (OR) efficiency.1 Extubation time is of special interests to surgeons and anesthesiologists because it could be affected by different anesthetic agents or techniques.2-4 Prolonged extubation decreases OR efficiency and causes slowing of work flow, having OR members staying idly waiting for extubation, and surgeons have to wait longer for next operation, but they always want patients quick to awaken.5 Accordingly, choosing appropriate anesthetics or techniques to avoid prolonged extubation is essential for anesthesiologists in order to improve the efficiency of OR. Dexter and Epstein6 recommended that recording extubation time and monitoring the incidence of prolonged extubation were very important especially at facilities that had at least 8 hours of cases and turnovers, and that prolonged extubation was defined as extubation time equal or longer than 15 minutes.7 Previous studies also implied that longer-than-average anesthesia times strongly influenced the academic anesthesiology departments by increasing the staffing costs and decreasing hourly productivity.8,9 The ACT between propofol-based total intravenous anesthesia (TIVA) and desflurane (DES) anesthesia in different surgeries was investigated; nevertheless, the results were controversial.4,10-18
Previous reports showed that hepatectomy may alter the pharmacodynamics of anesthetics and result in delayed recovery from propofol-based TIVA and inhalation anesthesia.19,20 Abou Hussein et al.21 reported that desflurane anesthesia provided faster extubation time compared with sevoflurane anesthesia in major liver resection. As our best knowledge, however, we found no rigorous comparisons between propofol-based TIVA and desflurane anesthesia for the improvement of ACT in open liver resection under general anesthesia (GA). Moreover, different propofol delivery techniques such as target-controlled infusion (TCI) and syringe pump infusion were used in these studies and might lead to different results. The aim of our present study was to determine whether the use of TIVA with TCI system is more effective than DES anesthesia in reducing ACT in patients undergoing open liver resection.
Methods
This retrospective study was approved by the Ethics Committee (TSGHIRB No. 100-05-168) of Tri-Service General Hospital, Taipei, Taiwan (Chairperson, Professor Pauling Chu) on 29th of August, 2011. Institutional Review Board allowed waiving the requirement for obtaining informed consent and patient records was anonymized and de-identified prior to analysis. The information was retrieved from the medical records and the electronic database of Tri-Service General Hospital (TSGH, Taipei, Taiwan). We enrolled 143 hepatocellular carcinoma patients (American Society of Anesthesiology [ASA] class I–III) who received elective open liver resection under TIVA with TCI or DES anesthesia from January 2010 to December 2011. Exclusion criteria included body mass index (BMI) > 35 kg/m2, emergent surgeries, patient younger than 18 years, combined TIVA with inhalation anesthesia or epidural anesthesia, other inhalation anesthesia besides desflurane, patients sent to the intensive care unit, or incomplete data. For the purposes of this study, the following times (minutes) were calculated: waiting for anesthesia time, arrival in the OR to anesthesia was introduced; surgical time, incision to surgical completion and application of dressings; anesthesia time, start of anesthesia to extubation; extubation time, from the end of skin closure until extubation; total OR stay time, arrival in the OR to departure from the OR; post-anesthesia care unit (PACU) stay time, arrival in the PACU to discharge from the PACU to the general ward; and ACT, arrival in the OR to discharge from the OR. In addition, other parameters included demographic data and ASA physical status.
There was no premedication before induction of anesthesia. Regular monitoring, such as noninvasive blood pressure, arterial line, electrocardiography (lead II), pulse oximetry, end-tidal carbon dioxide (EtCO2), radial arterial line monitoring, and a central venous catheter were applied in each patient. Anesthesia was induced with fentanyl and propofol in all patients. The patients were then intubated and maintained with propofol or DES and the analgesic fentanyl. In our common practice, we took patients to the PACU after extubation and did not extubate in PACU.
In the TIVA group, anesthesia was induced using IV fentanyl (2 µg/kg) and 2% lidocaine (1.5 mg/kg). Continuous infusion of propofol (Fresfol 1%) was delivered subsequently using Schneider’s kinetic model of TCI (Fresenius Orchestra Primea, Fresenius Kabi AG, Bad Homburg, Germany) with the effect-site concentration (Ce) of 4 µg/mL. Rocuronium (0.6 mg/kg, IV) was administered when patients lost consciousness, followed by tracheal intubation. Anesthesia was maintained using TCI with propofol Ce 3–4 µg/mL and an oxygen flow of 300 mL/min. Repetitive IV bolus injections of cisatracurium and fentanyl were prescribed as required throughout the procedure.12-18,22-25
In the DES group, the patients were induced with IV fentanyl (2 µg/kg), 2% lidocaine (1.5 mg/kg), and propofol (1.5–2 mg/kg). When patients lost consciousness, 0.6 mg/kg of rocuronium IV was administered, followed by endotracheal intubation. Anesthesia was maintained using 8–12% desflurane (inhaled Ce) in an oxygen flow of 300 mL/min under a closed system without nitrous oxide. Repetitive IV bolus injections of cisatracurium and fentanyl were prescribed as required throughout the procedure.12-18,22-24
Maintenance of the Ce for the TCI with propofol and DES Ce was adjusted at the range of 0.2 µg/mL and 0.5%, respectively, according to the hemodynamics. If two increments or decrements were unsuccessful, the range of Ce for TCI propofol and desflurane was increased to 0.5 µg/mL or 2%, respectively. The EtCO2 pressure was maintained at 35–45 mmHg by adjusting the ventilation rate and maximum airway pressure. Once neuromuscular function returns, cisatracurium (2 mg, IV) was administered as required.12-18,22-24
Ce of propofol or DES Ce was tapered to 2.0 µg/mL or 5% respectively at the beginning of skin closure. At the last five stitches of surgery, propofol or DES was discontinued, but the oxygen flow was kept 300 mL/min. At the end of the skin closure, the lungs were ventilated with 100% oxygen at a fresh gas flow of 6000 mL/min. Reversal of neuromuscular function was achieved by administrating neostigmine (0.03–0.04 mg/kg, IV) with glycopyrrolate (0.006–0.008 mg/kg, IV) once spontaneous breathing returned to prevent residual paralysis. When the patient regained consciousness by name with spontaneous and smooth respiration, the endotracheal tube was removed and the patient was sent to the PACU for further care.
Data are presented as the mean and SD, number of patients, or percentage. Demographic and perioperative variables were compared using Student’s t-test. Categorical variables were compared using chi-square test. Multivariable logistic regression analyses were performed to assess the association between variables contributed to prolonged extubation. The level of statistical significance was determined as P < 0.05. Statistical analyses were done using SPSS software version 21.0 (IBM Corp., Armonk, NY, USA).
Results
Thirty-eight patients were excluded from the analysis: 15 patients received sevoflurane anesthesia, 12 patients received combined inhalation anesthesia with propofol, 8 patients with incomplete data, and 3 patients had BMI > 35 kg/m2 (Figure 1).
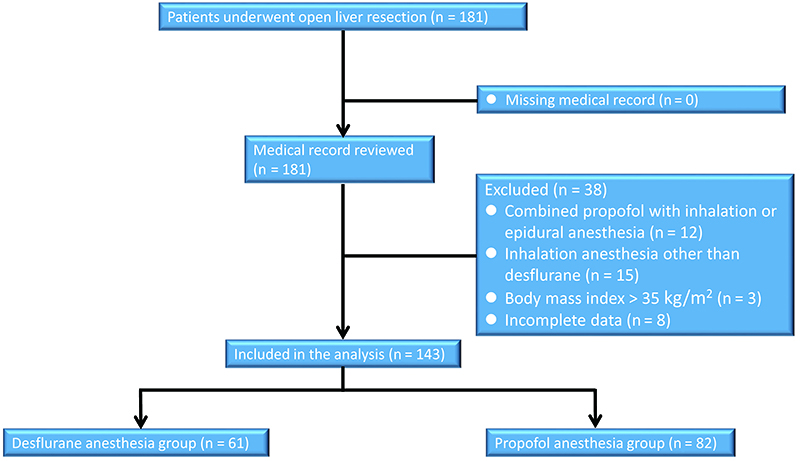
Download full-size image
Our study included 143 patients, of which 82 received TIVA and 61 received DES anesthesia. There was no significant difference in patient’s demographics (Table 1). The extubation time was faster in the DES group than in the TIVA group (10.1 ± 3.2 min vs. 11.8 ± 5.2 min; P = 0.03). The incidence of prolonged extubation was significantly lower in the DES group than in the TIVA group (9.8% vs. 26.8%; P = 0 .02). The waiting for anesthesia time, surgical time, anesthesia time, exit from OR after extubation, total OR time, and PACU time were no difference between groups (Table 2). In addition, the consumption of opioids and non-depolarizing muscle relaxants (NDMRs) were significantly higher in the TIVA group (Table 2).
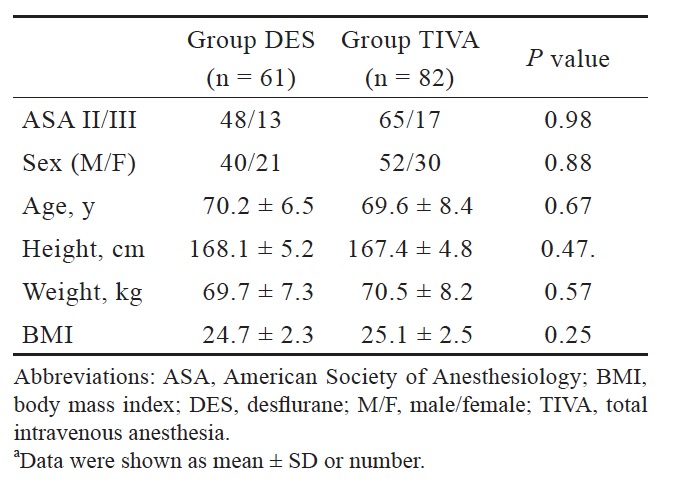
Download full-size image
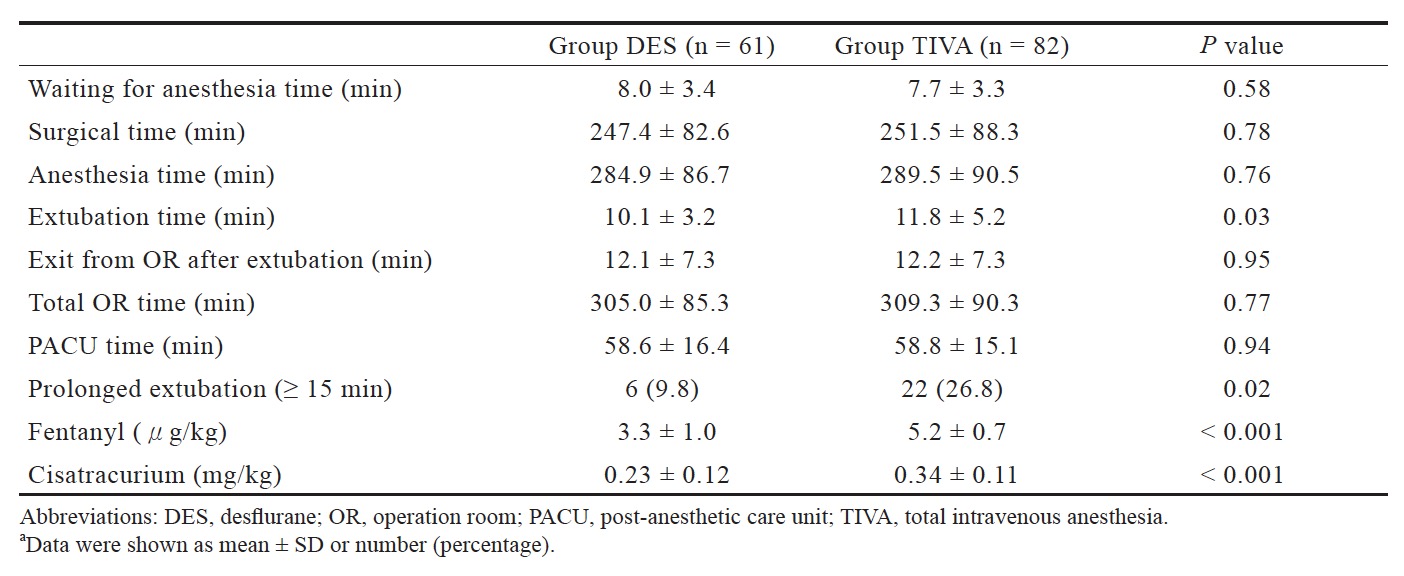
Download full-size image
The result of multivariable logistic regressions comparing prolonged extubation time between several variants in all patients was shown in Table 3. Age, sex, anesthetic technique, and anesthesia time were factors that contribute to extubation time. And the results showed that patients with older age, male, TIVA, and lengthy anesthesia time have longer extubation time.
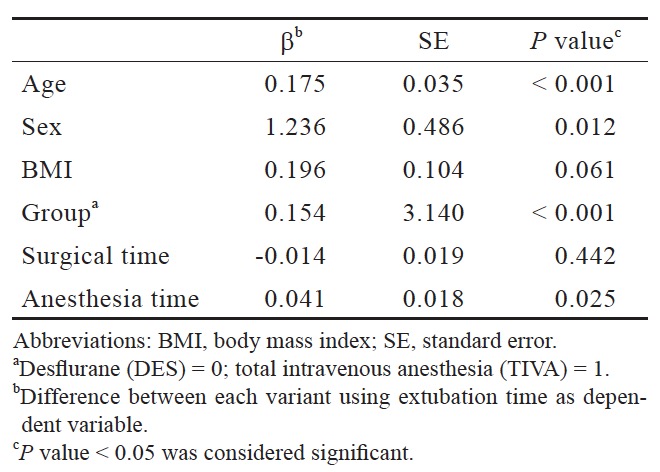
Download full-size image
Discussion
The major findings in this retrospective study showed that propofol-based TIVA by TCI significantly increased the extubation time and the incidence of prolonged extubation relative to the DES anesthesia in patients undergoing elective open liver resection. In this study, we also found that prolonged extubation was affected by age, sex, anesthetic technique, and anesthesia time in patients undergoing elective open liver resection.
The results of previous studies comparing the extubation time of desflurane with propofol-based TIVA have been controversial.4,10-18 Some studies comparing desflurane with TIVA found no significant difference in terms of extubation.12,26-28 Our previous studies found the use of TIVA with TCI system was more effective than desflurane in reducing ACT,13-18,29 because the awakening time can be predicted by TCI system.30 However, liver resection may alter the pharmacodynamics of anesthetics and result in delayed recovery.19,20 Major liver resection is associated with hemodynamic, hepatic and renal changes as a result of the procedure, and that may delay recovery.21 Desflurane was found to preserve better the hemodynamic parameters and enhance recovery in major liver resection.21 In contrast, prolonged extubation in propofol anesthesia might result from propofol accumulation and redistribution from the fatty tissue and muscle to the plasma, which leads to delay recovery by using continuous infusion in adult.31 In addition, the consumption of opioid and NDMRs in the TIVA group was significantly higher than in the DES group during surgical periods. This is reasonable because volatile anesthetics may increase the potency of NDMRs32 and demonstrate synergistic effects with opioids.33 These medications also contribute to delayed extubation. Accordingly, the present result was opposite to our previous studies but consistent with other researches reporting that GA using desflurane anesthesia could achieve faster extubation than using propofol-based TIVA in different surgeries.4,10,11,34,35
McIntosh et al.36 revealed that each 5 minutes reduction in intraoperative time should be treated as reducing costs, and the reduction was approximately 20% larger than the cost per 5 minutes of OR time. However, the reduction of anesthesia related time in OR did not necessarily equal to improvement of OR productivity unless there were sufficient case-numbers to fill a workday. In our study, the extubation time was 1.7 minutes faster in the DES group with statistical significance. However, the reduction in ACT, as reported in our study, might not be sufficient to schedule additional operation and could be reasonably treated as having no economic benefit.37
Prolonged extubation would decrease OR efficiency and occurred in 15% of all cases.3,38 In this study, the incidence of prolonged extubation in DES group was 9.8%, which was consistent with our previous study in open major upper abdominal surgery.13 From another point of view, the incidence of prolonged extubation in the TIVA group was 26.8%, which was higher than previous studies.3,6,13,38 Therefore, monitoring the incidence of prolonged extubation was recommended as an economic measure for intraperitoneal procedures in upper abdomen.6
Previous researches showed that the risk factors of prolonged extubation includes prone position, prolonged surgical time, significant blood loss, larger volume of crystalloid, and colloid infusion.39,40 And, our previous studies reported that older age, male, lengthy anesthesia time, and higher BMI contributed to prolonged extubation in open major upper abdominal surgery and open colorectal surgery.12,13 In the present study, older age was a risk factor for prolonged extubation. It might be due to that weight of the human brain decreases by about 10% with age,41 and the gray matter decreases more than the white matter, which may be more sensitive to anesthetics. Besides, the decrease in renal and hepatic reserve in elderly patients may also prolong anesthetics metabolism.12 In this study, we also found that male was a risk factor for prolonged extubation. The reason might reflect a possible hormonal influence on the effect of hypnotic drugs, and further investigation was needed.Consistently, we also found that lenghty anesthesia time contributed to prolonged extubation in this study. During lengthy surgical procedures, higher than necessary propofol infusion levels may accumulate and be redistributed from the fatty tissue and muscle to the plasma, which leads to delayed recovery,29,31 even under TCI. Inhaled desflurane is also redistributed in the fatty tissue and muscle, and may delay emergence in cases where the anesthesia time is increased.29 Therefore, monitoring anesthetic depth to keep the hypnotic level within the recommended range may improve anesthetic delivery and postoperative recovery from relatively deep anesthesia.42 Accordingly, bispectral index (BIS) use is strongly recommended in patients with older age or prolonged surgial time (> 210 minutes).12,13
This study has some limitations. First, our study is a retrospective study. Considering comparability and standardization of study groups, a retrospective study may contribute to bias. Although the choice of anesthetic management was not randomly allocated but rather by the availability of the TCI devices, the results showed no difference in the characteristics of the patients between two groups. The study, performed under clinical conditions, reflects more precisely the clinical relevant benefit. Second, we did not compare the effect of body temperature on extubation time because hypothermia may delay awakening.43 However, in our cases, we used the patient warming system including fluid wariming kit and convective air warming system to keep their core temperature ≥ 35°C perioperatively. Third, we excluded patients with BMI > 35 kg/m2 because obesity may lead to prolonged extubastion,13,43 and it is the limitation in Schnider model of TCI machine. Fourth, we did not use BIS in our common practice. Our incidence of prolonged extubation was 19.5% similar with overall 19.3% reported by a previous study in 4–5 hours surgery;6 however, use of BIS in hepatectomy was still suggested. Fifth, information about blood transfusion was incomplete in our medical records. Previous studies have shown that significant blood loss and larger volume of crystalloid and colloid infusion contributes to prolonged extubation.39,40 However, in our clinical practice, the requirements of blood transfusion and fluid infusion were no significantly differences between the propofol-based TIVA and desflurane anesthesia in liver surgery.29 In conclusion, our results showed that propofol-based TIVA by TCI increased the mean time on extubation and increased the incidence of prolonged extubation relative to desflurane anesthesia in open liver resection. In addition, older age, male, TIVA, and lengthy anesthesia time were factors affecting prolonged extubation.
Author Contributions
Hou-Chuan Lai designed the study, conducted the study, and wrote the main manuscript text. Yi-Hsuan Huang helped data collection and analysis, and prepared the main manuscript text. Chueng-He Lu helped data collection and analysis. Nan-Kai Hung helped data collection and analysis. Chih-Shung Wong helped data collection and analysis, and approved the final manuscript. Zhi-Fu Wu designed the study, conducted the study, and wrote the main manuscript text.
Conflict of Interest
None.
Ethical Approval of Studies
The Ethics Committee of Tri-Service General Hospital (Taipei, Taiwan) (TSGHIRB No. 100-05-168) approved the study (tsghirb@ndmctsgh.edu.tw).
Funding
None.
References
| 1 |
Junger A, Klasen J, Hartmann B, et al.
Shorter discharge time after regional or intravenous anaesthesia in combination with laryngeal mask airway compared with balanced anaesthesia with endotracheal intubation.
Eur J Anaesthesiol. 2002;19(2):119-124.
|
| 2 |
Apfelbaum JL, Grasela TH, Hug CC Jr, et al.
The initial clinical experience of 1819 physicians in maintaining anesthesia with propofol: characteristics associated with prolonged time to awakening.
Anesth Analg. 1993;77(4 suppl):S10-S14.
|
| 3 |
Dexter F, Bayman EO, Epstein RH.
Statistical modeling of average and variability of time to extubation for meta-analysis comparing desflurane to sevoflurane.
Anesth Analg. 2010;110(2):570-580.
|
| 4 |
Wachtel RE, Dexter F, Epstein RH, Ledolter J.
Meta-analysis of desflurane and propofol average times and variability in times to extubation and following commands.
Can J Anaesth. 2011;58(8):714-724.
|
| 5 |
Vitez TS, Macario A.
Setting performance standards for an anesthesia department.
J Clin Anesth. 1998;10(2):166-175.
|
| 6 |
Dexter F, Epstein RH.
Increased mean time from end of surgery to operating room exit in a historical cohort of cases with prolonged time to extubation.
Anesth Analg. 2013;117(6):1453-1459.
|
| 7 |
Agoliati A, Dexter F, Lok J, et al.
Meta-analysis of average and variability of time to extubation comparing isoflurane with desflurane or isoflurane with sevoflurane.
Anesth Analg. 2010;110(5):1433-1439.
|
| 8 |
Abouleish AE, Prough DS, Whitten CW, Conlay LA.
Increasing the value of time reduces the lost economic opportunity of caring for surgeries of longer-than-average times.
Anesth Analg. 2004;98(6):1737-1742.
|
| 9 |
Abouleish AE, Prough DS, Zornow MH, et al.
The impact of longer-than-average anesthesia times on the billing of academic anesthesiology departments.
Anesth Analg. 2001;93(6):1537-1543.
|
| 10 |
Juvin P, Servin F, Giraud O, Desmonts JM.
Emergence of elderly patients from prolonged desflurane, isoflurane, or propofol anesthesia.
Anesth Analg. 1997; 85(3):647-651.
|
| 11 |
Gupta A, Stierer T, Zuckerman R, Sakima N, Parker SD, Fleisher LA.
Comparison of recovery profile after ambulatory anesthesia with propofol, isoflurane, sevoflurane and desflurane: a systematic review.
Anesth Analg. 2004;98(3):632-641.
|
| 12 |
Chan WH, Lee MS, Lin C, et al.
Comparison of anesthesia-controlled operating room time between propofol-based total intravenous anesthesia and desflurane anesthesia in open colorectal surgery: a retrospective study.
PLoS One. 2016;11(10):e0165407.
|
| 13 |
Lai HC, Chan SM, Lu CH, Wong CS, Cherng CH, Wu ZF.
Planning for operating room efficiency and faster anesthesia wake-up time in open major upper abdominal surgery.
Medicine (Baltimore). 2017;96(7):e6148.
|
| 14 |
Lai HC, Hung NK, Lin BF, Chen JL, Huang YH, Wu ZF.
Lower incidence of prolonged extubation in propofol-based total intravenous anesthesia compared with desflurane anesthesia in laparoscopic cholecystectomy: a retrospective study.
J Med Sci. 2019;39(3):121-126.
|
| 15 |
Wu ZF, Jian GS, Lee MS, et al.
An analysis of anesthesia-controlled operating room time after propofol-based total intravenous anesthesia compared with desflurane anesthesia in ophthalmic surgery: a retrospective study.
Anesth Analg. 2014;119(6):1393-1406.
|
| 16 |
Lu CH, Wu ZF, Lin BF, et al.
Faster extubation time with more stable hemodynamics during extubation and shorter total surgical suite time after propofol-based total intravenous anesthesia compared with desflurane anesthesia in lengthy lumbar spine surgery.
J Neurosurg Spine. 2016;24(2):268-274.
|
| 17 |
Lai HC, Chan SM, Lin BF, Lin TC, Huang GS, Wu ZF.
Analysis of anesthesia-controlled operating room time after propofol-based total intravenous anesthesia compared with desflurane anesthesia in gynecologic laparoscopic surgery: a retrospective study.
J Med Sci. 2015;35(4):157-161.
|
| 18 |
Liu TC, Lai HC, Lu CH, et al.
Analysis of anesthesia-controlled operating room time after propofol-based total intravenous anesthesia compared with desflurane anesthesia in functional endoscopic sinus surgery.
Medicine (Baltimore). 2018;97(5):e9805.
|
| 19 |
Murata F, Iwade M, Hidano G, Tsunoda C, Nagata O, Ozaki M.
Recovery from propofol anesthesia is delayed in hepatectomy patients due to altered pharmacodynamics.
Masui. 2006;55(2):150-157. [In Japanese]
|
| 20 |
Murata F, Iwade M, Nagata O, Ozaki M.
Recovery from sevoflurane anesthesia delayed in hepatectomy patients due to influence of operation.
Masui. 2007;56(6):650-656. [In Japanese]
|
| 21 |
Abou Hussein M, Mahmoud F, Beltagy R, Hasanin A, Yassen K, Attar A.
Desflurane compared to sevoflurane for cirrhotic patients undergoing major liver resection. A randomized control study.
Middle East J Anaesthesiol. 2015;23(2):213-223.
|
| 22 |
Wu ZF, Lee MS, Wong CS, et al.
Propofol-based total intravenous anesthesia is associated with better survival than desflurane anesthesia in colon cancer surgery.
Anesthesiology. 2018;129(5):932-941.
|
| 23 |
Lai HC, Pao SI, Huang YS, Chan SM, Lin BF, Wu ZF.
The Relationship between postoperative pneumonia and endotracheal suctioning under general anesthesia in ophthalmic surgery: a retrospective study.
Asian J Anesthesiol. 2018;56(1):33-38.
|
| 24 |
Lai HC, Tseng WC, Pao SI, et al.
Relationship between anesthesia and postoperative endophthalmitis: a retrospective study.
Medicine (Baltimore). 2017; 96(12):e6455.
|
| 25 |
Hung NK, Lee MS, Lai HC, et al.
Optimal effect-site concentration of propofol for tracheal suctioning during emergence from ophthalmic surgery.
Medicine (Baltimore). 2020;99(1):e18669.
|
| 26 |
Grundmann U, Silomon M, Bach F, et al.
Recovery profile and side effects of remifentanil-based anaesthesia with desflurane or propofol for laparoscopic cholecystectomy.
Acta Anaesthesiol Scand. 2001;45(3):320-326.
|
| 27 |
Fombeur PO, Tilleul PR, Beaussier MJ, Lorente C, Yazid L, Lienhart AH.
Cost-effectiveness of propofol anesthesia using target-controlled infusion compared with a standard regimen using desflurane.
Am J Health Syst Pharm. 2002;59(14):1344-50.
|
| 28 |
Mahli A, Coskun D, Karaca GI, Akcali DT, Karabiyik L, Karadenizli Y.
Target-controlled infusion of remifentanil with propofol or desflurane under bispectral index guidance: quality of anesthesia and recovery profile.
J Res Med Sci. 2011;16(5):611-620.
|
| 29 |
Lu CH, Yeh CC, Huang YS, et al.
Hemodynamic and biochemical changes in liver transplantation: a retrospective comparison of desflurane and total intravenous anesthesia by target-controlled infusion under auditory evoked potential guide.
Acta Anaesthesiol Taiwan. 2014;52(1):6-12.
|
| 30 |
Chan SM, Lee MS, Lu CH, et al.
Confounding factors to predict the awakening effect-site concentration of propofol in target-controlled infusion based on propofol and fentanyl anesthesia.
PLoS One. 2015;10(5):e0124343.
|
| 31 |
Levitt DG, Schnider TW.
Human physiologically based pharmacokinetic model for propofol.
BMC Anesthesiol. 2005;5(1):4.
|
| 32 |
Paul M, Fokt RM, Kindler CH, Dipp NC, Yost CS.
Characterization of the interactions between volatile anesthetics and neuromuscular blockers at the muscle nicotinic acetylcholine receptor.
Anesth Analg. 2002;95(2):362-367.
|
| 33 |
Hendrickx JFA, Eger EI 2nd, Sonner JM, Shafer SL.
Is synergy the rule? A review of anesthetic interactions producing hypnosis and immobility.
Anesth Analg. 2008;107(2):494-506.
|
| 34 |
Yu H, Zhang L, Ma Y, Yu H.
Early postoperative recovery in operating room after desflurane anesthesia combined with Bispectral index (BIS) monitoring and warming in lengthy abdominal surgery: a randomized controlled study.
BMC Anesthesiol. 2018;18(1):110.
|
| 35 |
Dolk A, Cannerfelt R, Anderson RE, Jakobsson J.
Inhalation anaesthesia is cost-effective for ambulatory surgery: a clinical comparison with propofol during elective knee arthroscopy.
Eur J Anaesthesiol. 2002;19(2):88-92.
|
| 36 |
McIntosh C, Dexter F, Epstein RH.
The impact of service-specific staffing, case scheduling, turnovers, and first-case starts on anesthesia group and operating room productivity: a tutorial using data from an Australian hospital.
Anesth Analg. 2006;103(6):1499-1516.
|
| 37 |
Dexter F, Macario A.
Decrease in case duration required to complete an additional case during regularly scheduled hours in an operating room suite: a computer simulation study.
Anesth Analg. 1999;88(1):72-76.
|
| 38 |
Masursky D, Dexter F, Kwakye MO, Smallman B.
Measure to quantify the influence of time from end of surgery to tracheal extubation on operating room workflow.
Anesth Analg. 2012;115(2):402-406.
|
| 39 |
Epstein RH, Dexter F, Brull SJ.
Cohort study of cases with prolonged tracheal extubation times to examine the relationship with duration of workday.
Can J Anaesth. 2013;60(11):1070-1706.
|
| 40 |
Li F, Gorji R, Tallarico R, et al.
Risk factors for delayed extubation in thoracic and lumbar spine surgery: a retrospective analysis of 135 patients.
J Anesth. 2014;28(2):161-166.
|
| 41 | |
| 42 |
Punjasawadwong Y, Phongchiewboon A, Bunchungmongkol N.
Bispectral index for improving anaesthetic delivery and postoperative recovery.
Cochrane Database Syst Rev. 2014;6:CD003843.
|
| 43 |
Kleine S, Hofmeister E, Egan K.
Multivariable analysis of anesthetic factors associated with time to extubation in dogs.
Res Vet Sci. 2014;97(3):592-596.
|