Abstract
Dystrophic epidermolysis bullosa (DEB) is a rare genetic skin disease characterized by blisters and ulcers on the skin and mucosa after minor friction. The risk of invasive squamous cell carcinoma on the unhealed ulcers increases with age. Tracheal intubation during general anesthesia may induce tracheal stricture due to blister formation and/or scarring in DEB patients and cause severe airway obstruction. There is no consensus for handling DEB patients’ fragile mucosa and skin during general anesthesia. We report an adult DEB patient who received two operations under different general anesthesia methods. The experience from this particular patient and her response to anesthesia may provide a satisfactory guide to avoid complications and improve the outcome for DEB patients receiving general anesthesia.
Keywords
dystrophic epidermolysis bullosa, general anesthesia, intubation
Introduction
Dystrophic epidermolysis bullosa (DEB) is an inherited severe bullous disease characterized by extreme skin fragility and blistering formation between the junction of dermis and epidermis in response to minor trauma.1 For anesthesiologists, it presents challenges of skin care, venous access establishing during anesthesia, as well as the scarring of skin and mucosa resulting in difficult intubation. We report a patient who received two different types of general anesthesia for skin surgeries. Our experience may provide possible guidance of modern anesthetic management for DEB patients.
Case Presentation
A 54-year-old lady was diagnosed with DEB since birth. She presented with many blisters and chronic ulcers over her occipital scalp, oral mucosa, shoulder, trunk, and extremities (Figure 1). She also had oral and pharyngeal blisters and poor dentition. She refused local anesthesia for her skin grafts from the scalp to improve multiple chronic skin ulcers on the shoulders because of the painful injections of local anesthetics. Her skin was very sensitive to pain, probably related to daily wound dressings since birth. The pre-anesthetic evaluation revealed anemia (hemoglobin level 10.1 g/dL). She was also a chronic hepatitis B carrier without an active flare-up. For airway evaluation, she suffered from limited mouth opening (< 2 fingerbreadth) due to oral mucosa scarring. There was also mild limited neck motion due to ulcers over the nape. The patient’s Mallampati classification was two, and the thyromental distance was around 6 cm. The major diffi culty of airway establishment was the scarring and blisters around her mouth, which limited her mouth opening. Although we decided to preserve her spontaneous breathing with intravenous anesthesia, we still prepared a lubricated direct laryngoscope and video stylet for the possible necessity of endotracheal tube intubation during induction. A laryngeal mask was also prepared for potential difficult airway. Non-invasive blood pressure monitoring, 3-lead electrocardiogram (ECG) and pulse oximeter were used during the operation. Her arm was wrapped with cotton before applying the cuff of noninvasive blood pressure monitoring to prevent shearing force-induced blisters. Thick lubricant jelly between the ECG electrodes and the skin was applied to avoid friction blisters. A pulse oximeter was placed on a suitable digit.
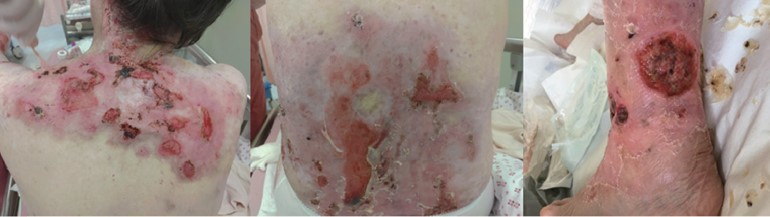
Download full-size image
The first operation was scheduled in November 2017. To manage skin grafts from her left occipital area to her upper back area for chronic ulcers, we asked her to lie in the right decubitus position. She was gently positioned before induction, and the pressure points were protected with soft protectors or gauze. A warm blanket was used to maintain adequate body temperature. The intravenous line was placed in her left dorsal hand. After pre-oxygenation for 3 minutes gently with face mask, intravenous fentanyl 25 mcg with 2% lidocaine 40 mg were given. General anesthesia was induced via target-controlled infusion with propofol. She lost her consciousness at the calculated effect site concentration (Ce) value of 2.5 ug/ mL. Only face mask technique was used as airway control, and spontaneous breathing was preserved. Eye ointment was applied to prevent corneal damage. Intermittent intravenous fentanyl 25 mcg was given to keep mean arterial pressure (MAP) range from 60 to 100 mmHg and to prevent movement. Her heart rate was kept within 60–80 beats per minute throughout the whole operation. There was no new blister formation during or after the operation. There was no nasal or oral airway placement throughout this surgery. The surgery took approximately four hours. She was transferred to a post-anesthetic recovery room and regained consciousness 15 minutes after discontinuation of propofol.
Seven months after her first procedure, she was scheduled for another skin grafting. This time, we chose combined intravenous and volatile anesthesia. We also lubricated her face with ointment and sealed the face mask with gauze bandage gently. Spontaneous breathing was maintained with a 2.5% sevoflurane volatile anesthetic throughout the procedure. After preparation and patient positioning, bolus intravenous fentanyl 25 mcg was given just before starting the surgery. Intravenous propofol was also given with a syringe pump and the rate ranged from 50 to 400 mg per hour. The rate was adjusted to avoid patient movement during the operation. MAP and heart rate were kept from 65 to 105 mmHg and 55 to 65 bpm, respectively. There was also no new blister formation during or after this operation. The second procedure took around four hours, too. The patient was transferred to the recovery room after the procedure. However, this time the patient experienced dizziness after emergence. Severe postoperative nausea and vomiting (PONV) developed and persisted for one day, which lowered her patient satisfaction with the second anesthesia experience.
Discussion
Epidermolysis bullosa (EB) is a group of genetic disorders that presented with blisters and ulcers of the skin and mucosa even after trivial shearing force. There are three main categories: EB simplex, junctional, and DEB. DEB can be inherited as an autosomal dominant or recessive trait.1 The age range of patients who received surgical procedures under anesthesia was reported mostly in the first and second decade, and the surgical procedures include wound dressing, syndactyly repair, esophageal dilatation, and skin grafts over the lesions.2
Pre-anesthetic assessment should pay attention to airway assessment plus the malnutrition secondary to esophageal stricture and limited mouth intake and possible electrolyte imbalance.3 Persisted catabolic condition, nutrition compromise, and various hemorrhagic lesions also contribute to chronic anemia.3-5 Using a face mask for airway management during general anesthesia in EB patients was the major method in previous reports. However, laryngeal mask and endotracheal tube were also reported without significant complications for new blister formation.6 Tracheal intubation could be performed orally by using a direct laryngoscope with a lubricated blade. Patients with a history of oral or pharyngeal scarring may cause limited mouth opening. Fiberscope should be prepared for potentially difficult intubation.7 Nasotracheal fiberoptic intubation, which could avoid the pressure of laryngoscope to the supraglottic area, was recommended as a good choice for patients with EB in some studies.5 Nevertheless, tracheal and bronchial mucosa, as well as oropharyngeal and laryngeal mucosa, could also be involved with EB. Trauma during airway management may lead to airway stenosis and subsequent tracheostomy or bronchial balloon dilatation.8 Therefore, careful preoperative airway evaluation of blister location and postoperative blister checking are important to keep the airway unobstructed.
Several suggestions were given if intubation happened. (1) Routine airway assessment is the first step, which includes neck motion assessment, mouth opening, thyromental distance, Mallampati classification, and upper lip bite test. (2) Examine the nasopharynx and oropharynx carefully and record the patient’s mucosal lesion and site of stricture. (3) Either lubricated direct laryngoscope or video-assisted device should be prepared and a suitable tool should be chosen according to individual situations. (4) If mask ventilation or intubation seems difficult for the patient, awaking fiberoptic intubation with thorough lubricant along the intubation pathway, from the nasopharynx to supraglottic area, could be considered. Gentle advancement of the shaft of fiberoptic scope and the tube is necessary. (5) A laryngeal mask should always be prepared for unexpected difficult intubation or mask ventilation.
Anesthetic techniques could be regional, general, or both. The general principle is “light touch, no friction.” Adhesive dressing is not recommended for EB patients.9 The positioning of the patient should be managed carefully. Regional anesthesia may be used successfully in particular situations. A report demonstrated successful management for a DEB patient who underwent percutaneous nephrolithotomy using the combined spinal-epidural technique.10 Some case reports showed uneventful correction of pseudosyndactyly with interscalene brachial plexus block.3 Adequate postoperative analgesia in the postanesthetic care unit is also important to prevent struggling and agitation during emergence and recovery.7 Opioids should be avoided to reduce the potential opioidinduced pruritus.7
In this report, we maintained spontaneous breathing with face mask ventilation to avoid the bullae formation associated with a laryngeal mask or endotracheal tube for skin graft operations. Prolonged surgery such as dental procedure or dilatation of esophageal stricture may need intubation to assure a stable airway. Ames et al. recommended that general anesthesia as the sole anesthetic instead of regional anesthesia for EB patients.6 This conclusion may need further justification in advanced anesthetic techniques nowadays. For our patient, only general anesthesia could be used but the patient experienced PONV after recovery from the second anesthesia. The main difference between these general anesthetic techniques was the usage of two different anesthetics. The eye care, skin care with the monitors set up, warming technique were similar. In previous case reports, volatile anesthesia was used in 61% cases for induction and maintenance of anesthesia and propofol was mostly used in total intravenous anesthesia.2 Volatile anesthesia is believed to be the major cause of developing early PONV.11 The risk of esophageal mucosa which eventually leads to scarring and stricture after severe vomiting in DEB patients is high. However, whether EB patients are more susceptible to develop PONV needs more studies to confirm.
In conclusion, detailed pre-anesthetic assessment, team-based approach, and coordination between dermatologist, surgeon, nurse and anesthesiologist are keys to prevent iatrogenic harm and avoid complications in DEB patients who need procedures in an operating room.
Acknowledgments
The study was supported by the Center of Applied Nanomedicine, National Cheng Kung University from the Featured Areas Research Center Program within the framework of the Higher Education Sprout Project by the Ministry of Education (MOE) in Taiwan to T.W.W. We sincerely thank Dr. Rosie Hsu for her suggestions to the manuscript.
Financial Disclosure
None.
Conflict of Interest
None.
References
| 1 |
Baloch MS, Fitzwilliams B, Mellerio J, Lakasing L, Bewley
S, O’Sullivan G.
Anaesthetic management of two different modes of delivery in patients with dystrophic epidermolysis bullosa.
Int J Obstet Anesth. 2008;17(2):153-158.
|
| 2 |
Griffin RP, Mayou BJ.
The anaesthetic management of patients with dystrophic epidermolysis bullosa. A review of 44 patients over a 10 year period.
Anaesthesia. 1993;48(9):810-815.
|
| 3 |
Hagen R, Langenberg C.
Anaesthetic management in patients with epidermolysis bullosa dystrophica.
Anaesthesia. 1988;43(6):482-485.
|
| 4 |
Tomlinson AA.
Recessive dystrophic epidermolysis bullosa. The anaesthetic management of a case for major surgery.
Anaesthesia. 1983;38(5):485-491.
|
| 5 |
Lindemeyer R, Wadenya R, Maxwell L.
Dental and anaesthetic management of children with dystrophic epidermolysis bullosa.
Int J Paediatr Dent. 2009;19(2):127-134.
|
| 6 |
Ames WA, Mayou BJ, Williams K.
Anaesthetic management of epidermolysis bullosa.
Br J Anaesth. 1999;82(5):746-751.
|
| 7 | |
| 8 |
Arya R, Boujaoude Z, Gratz I, Akers S, Abouzgheib W.
Bronchial stenosis secondary to epidermolysis bullosa successfully treated with bronchoscopic balloon dilatation.
Respirol Case Rep. 2015;3(1):33-35.
|
| 9 |
Siddiqui KM, Khan S.
Anaesthetic management of an infant with epidermolysis bullosa undergoing inguinal hernia repair.
J Pak Med Assoc. 2010;60(6):497-498.
|
| 10 |
Nguyen L, Minville V, Riu B, Atallah F, Fourcade O.
Anaesthetic management of a patient with epidermolysis bullosa undergoing percutaneous nephrolithotomy.
Eur J Anaesthesiol. 2005;22(7):558-560.
|
| 11 |
Apfel CC, Kranke P, Katz MH, et al.
Volatile anaesthetics may be the main cause of early but not delayed postoperative vomiting: a randomized controlled trial of factorial design.
Br J Anaesth. 2002;88(5):659-668.
|